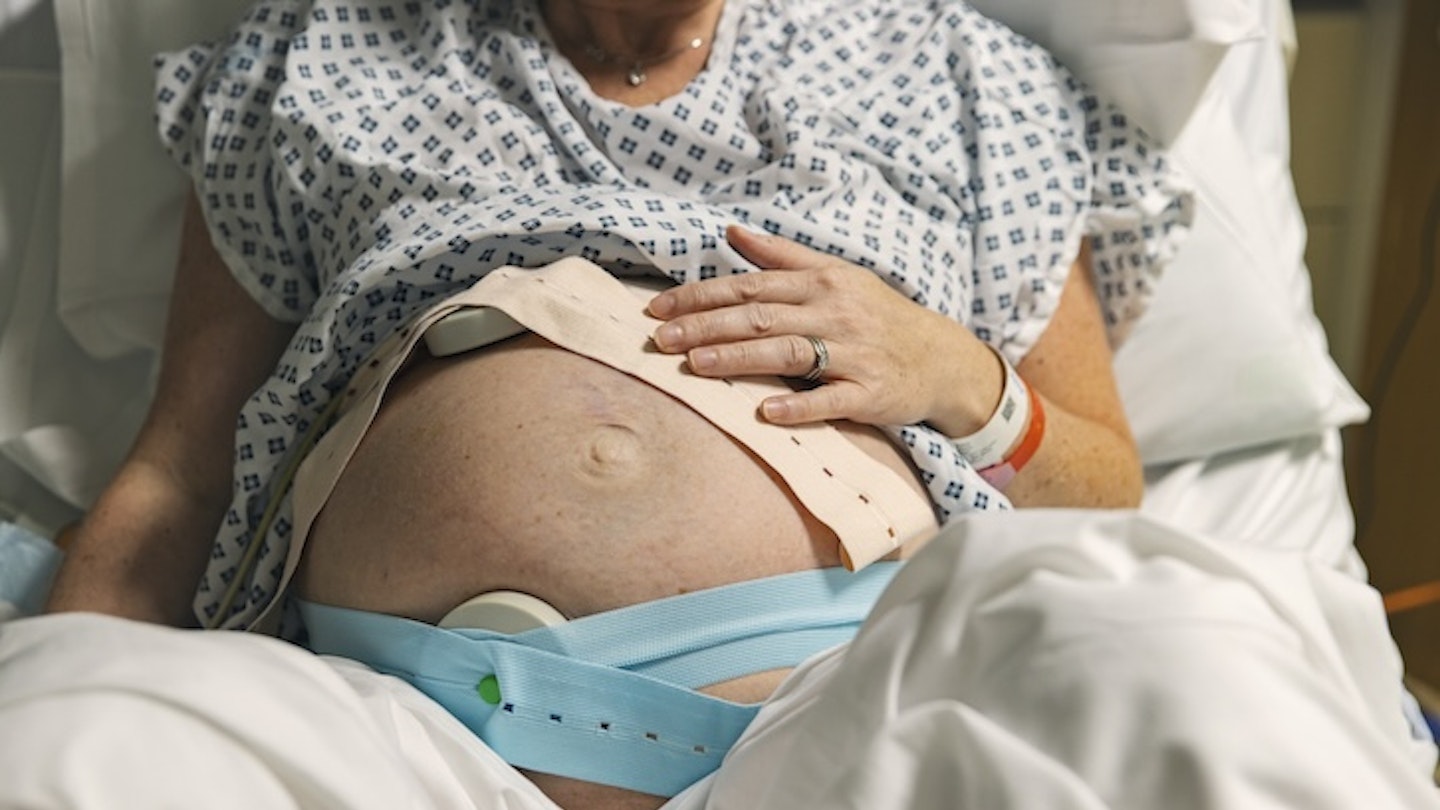
Some words make such an impact that they’re impossible to forget. In my case, they came from a nurse who was persuading me to be induced after my waters broke before my daughter Emilia’s birth, while I wanted to ask a doctor for a C-section. ‘The longer you wait, the more chance there is that your baby will die,’ she warned. With that, I felt I had no choice and agreed to be induced. During the delivery, Emilia’s shoulders got stuck (shoulder dystocia) and they had five minutes to get her out – I was terrified we’d lose her. Thankfully, a manoeuvre worked quickly and she was born unharmed.
But when learning about shoulder dystocia later, I realised the only risk factor that applied to us was being induced. It felt like I’d made the wrong call and, five years on, I still carry that guilt.
I’m one of thousands of women who have a traumatic birth in the UK each year, women who are often left dealing with physical and mental scars. According to the Birth Trauma Association, up to 30,000 women a year develop post-traumatic stress disorder (PTSD) after birth, and as many as 40% find part of birth traumatic, says Dr Rebecca Moore from Make Birth Better. Standards in maternity care seem to be slipping, with a report from the Care Quality Commission (CQC) last November deeming two-thirds (67%) of maternity units in England unsafe compared with 55% the previous year.
‘Often, the main cause of trauma wasn’t what went wrong in the birth, but how women felt badly treated – their pain and suffering was minimised, they weren’t listened to and were sometimes even laughed at or shouted at,’ says Kim Thomas from the Birth Trauma Association.
Gabriela Rye, 40, knows this all too well. She got a third-degree tear during the birth of her son, now seven, which went unnoticed and left her with faecal incontinence. She had always wanted a water birth at home with no interventions, but ended up being induced in hospital and asking for an epidural. A doctor used forceps and she lost a lot of blood.
As a midwife stitched her up, Gabriela asked her how bad it was. ‘She said I had a second-degree tear. I asked her three times if she was sure and if she’d checked me thoroughly. I felt so unwell that, in my head, I said goodbye to everyone because I felt I was dying. Then, as I turned purple, they realised I’d lost a lot of blood and I had a blood transfusion. I’d lost two pints.’
Despite repeatedly raising concerns with midwives and GPs in the following days and weeks, it wasn’t until six months later that a doctor finally realised Gabriela had a third-degree tear. By then, it was too late to repair it. ‘It was so traumatic to find out I had no control over my bowels and there was nothing they could do,’ recalls Gabriela. ‘If it had been spotted at the birth it would have been stitched up and I’d be fine. After that I was depressed and angry. I was let down by the people I had to trust were doing the right thing for me.’
‘During a good birth, people feel safe and heard,’ says Moore. ‘But we’ve got maternity teams that are understaffed, under-resourced and relentlessly busy and they’re too stretched to give the compassionate care people need. People want to trust doctors and midwives but they often end up feeling powerless, uninformed and unable to ask questions. Then they blame themselves.’
There is often a feeling that birth would be different if men had children. ‘There is a lot of misogyny in healthcare and we know female health has a lot of gaslighting and shame around it,’ says Illiyin Morrison, a midwife and author of The Birth Debrief. ‘It’s often men making decisions as to where the money goes in care, so perhaps things would be better if they were the ones to give birth.’
Illiyin, who was advised to have an emergency C-section rather than the home birth she wanted, felt dismissed during the birth of her daughter Ihsan, now five. ‘When I asked to explore other options, the doctor was very dismissive and slammed the door. They weren’t listening to me and it felt like I had no agency in the situation, even though, as a midwife, I had a visible understanding of what was happening. Things like that exacerbated my feelings of disappointment and upset after her birth and I found the transition to motherhood difficult.’
Illiyin adds that things are often even worse for Black, mixed-race and Asian women. ‘Black women are four times more likely to die in pregnancy or childbirth than white women – if that’s the rate of dying, what are the rates of the trauma we are experiencing? Other than underlying health conditions, the main reason for this is racism and unconscious bias.’
Robyn Frame, 36, blamed herself for her son Jude’s traumatic birth. She agreed to a VBAC (vaginal birth after Caesarean) after a doctor reassured her that her baby’s heart rate would be monitored once labour started. But when the time came, no one listened to her saying it needed to be done. Jude’s heart was only monitored when Robyn was almost fully dilated, and they realised then that his heart rate was very low and he was struggling, so Robyn ended up needing an emergency C-section under general anaesthetic. ‘I woke up not knowing if he was alive,’ she says. Afterwards, she says, ‘I blamed myself, thinking I should have had a scheduled C-section rather than a VBAC.’
So how can things improve? Moore says there needs to be better ways to assess and support women with trauma more quickly after birth and give women spaces to talk about their births. ‘Trauma symptoms often peak six to 12 months afterwards. There are some specialist services but they’re very unequal across the country,’ she says. Doctors agree things need to change. ‘The inescapable truth is that maternity services are under severe strain,’ says Dr Ranee Thakar, president of the Royal College of Obstetricians and Gynaecologists. ‘There’s need for investment in maternity staffing and training, and to work together to improve care. Most women in the UK give birth safely without trauma, but there’s room for improvement and we need to better prepare women for the unexpected. Our ultimate aim is to have a healthy mother and baby.’
For help and support visit: makebirthbetter.org; birthtraumaassociation.org; birthrights.org.uk; _masic._org.uk.