This week marks the 70th anniversary of the National Health Service – an institution at the heart of British identity. Grazia’s Anna Silverman spends the day with an NHS nurse...
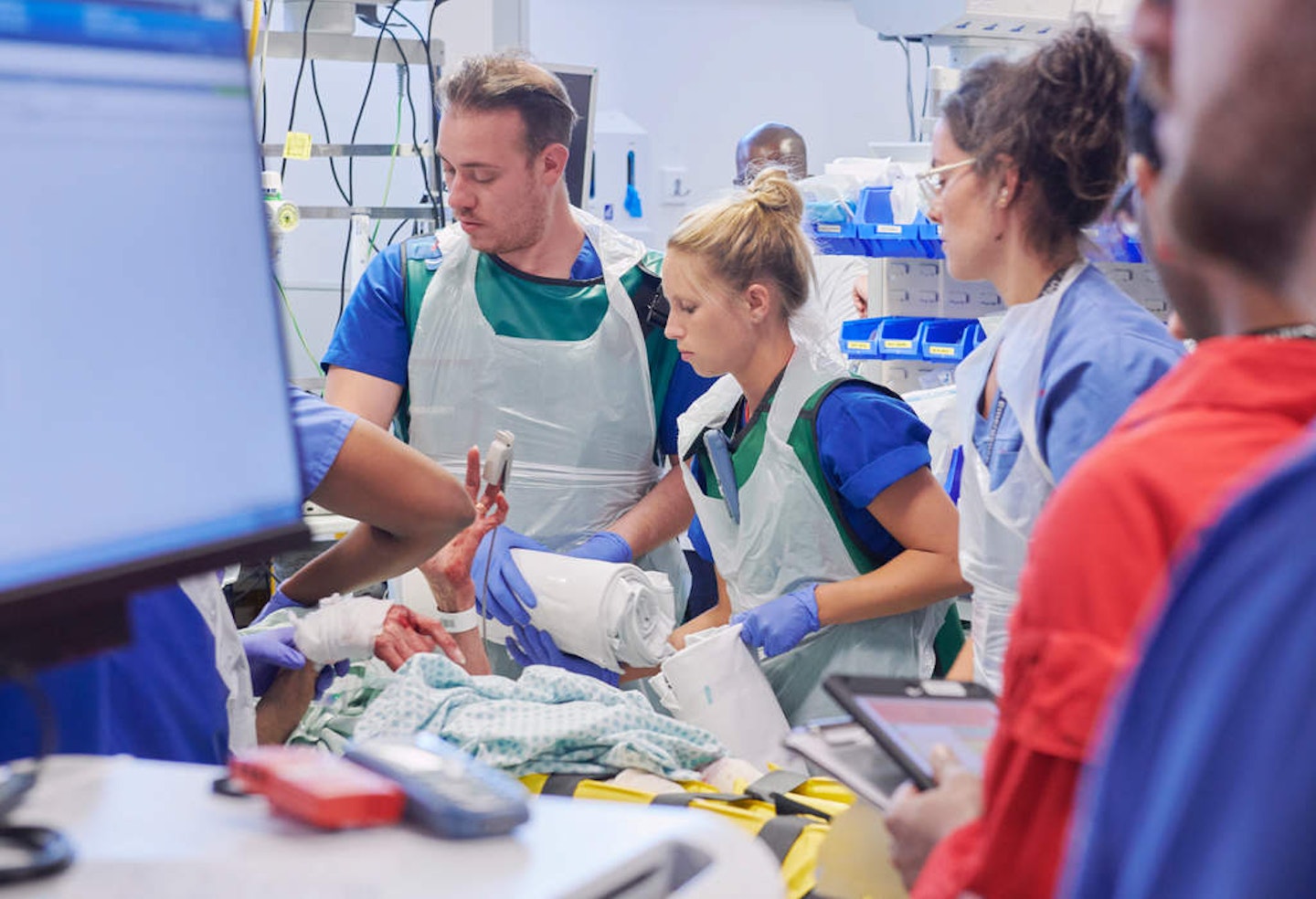
It’s 11am on a Tuesday in the Royal London Hospital and 20 nurses and doctors are pouring into the resuscitation ward in A&E. They’ve all received the ‘code red trauma’ alarm on their bleepers to tell them an 85-year-old woman has been run over and is on the helipad after being airlifted in.
Moments later, the patient – Daphne Francis – is wheeled through; her blood- drenched hands are trembling. Medics surround her and the nurse in charge, Holly Moore, takes her blood pressure and makes her comfortable.
A few beds down lies a two-year-old girl with lung problems, clutching a teddy. She’s struggling to breathe and her mother is fraught as another group of doctors and nurses crowd around her.
This is a typical morning in A&E at The Royal London – which can see as many as 627 trauma calls in 24 hours. Grazia has been given unrestricted access to witness a day in the life of a nurse here, to mark the 70-year anniversary of the NHS.
Holly, 32, is the nurse in charge today, which makes her responsible for 10 departments and up to 100 patients in A&E. She’s been a nurse for 10 years, six of which have been at this hospital. It’s a job she’s passionately proud to do but one that, inevitably, comes with difficulties.
‘It’s stressful trying to stick to the Government’s target of seeing and discharging patients within four hours, as our priority is making sure they’re safe and getting good care,’ she says. ‘It’s especially hard when there’s overcrowding and no beds available, which happens in every A&E across the country.’
Holly believes the key to improving healthcare lies in increasing services in primary care, like GPs. She’s tired of the relentless bashing the NHS gets in the media. ‘It’s difficult to hear,’ she adds. ‘When you look at countries like America and see their health service you realise how lucky we are here. I wish people appreciated it more.’
Has she noticed many changes in her 10 years? ‘Patient volume has increased, which brings with it more pressures. There are more violent crimes now, too – a lot more stabbings.’ By midday she’s already attended to one stab victim – a man in his twenties who groans as he’s brought in with two wounds to the back and one to the stomach.
Simultaneously, a car crash victim is rushed in: a 61-year-old woman who, a medic from the London Ambulance Service announces, is ‘injured from top to toe’. Holly quickly goes about preparing the medicines the patient will need.
By 3.30pm she still hasn’t sat down or eaten. Is this normal? She smiles and nods. She’s in by 7.20am and can clock up to 10km in steps by the time she finishes at 8.15pm. Yet she can’t imagine doing a more rewarding job. The only way to survive, however, is with a strong support network around her from colleagues.
Recently, a baby died, so her team rallied together to support one another and share how they were feeling. She’s hit by emotion the most when she has to break bad news to families. ‘I can be calm during the trauma call and then I see the family’s distress and it brings it home – especially when I’m telling a parent their child has died, or a husband or wife their partner hasn’t made it.’
Later that day, I return to 85-year-old Daphne. She’s stable now and going under general anaesthetic for an operation soon. She tells me that, from 1952 to 1969 she, too, was an NHS nurse.
‘It makes me proud to see nurses carrying on what we started all those years ago. It’s changed, of course. We had to sterilise everything and now it’s all disposable. We didn’t have anything hi-tech in my day,’ she laughs as a mobile X-ray system swoops over her head on a rail.
Holly tucks a blanket around her feet and dabs the former nurse’s parched mouth with water, as Daphne adds: ‘I just hope the NHS never goes private. Like today, if anything happens to me, I always know I’m in safe hands.’
