The coronavirus disease 2019 (COVID-19) pandemic is having a significant impact on all our lives and it is clear that while we are living in a ‘new normal’, one thing remains the same – cancer does not wait.
For those women (and men) worried about breast cancer or indeed with a recent diagnosis of breast cancer requiring treatment, this time has been even more difficult. At the start of the pandemic the UK government advice was to stay home and ‘protect the NHS’. The NHS came under severe strain looking after patients with COVID-19 but we also managed to keep essential cancer services running, and to ensure the safety of those needing treatment.
However, from necessity, with staff numbers limited due to sickness or redeployment to other areas within hospitals, the usual diagnostics and treatment pathways have differed from usual, and with the second wave now upon us cancer pathways will remain different for some time.
Despite the challenges of COVID, for women who have any concerns about their breast health or are looking for support, there are two things it's important to know.
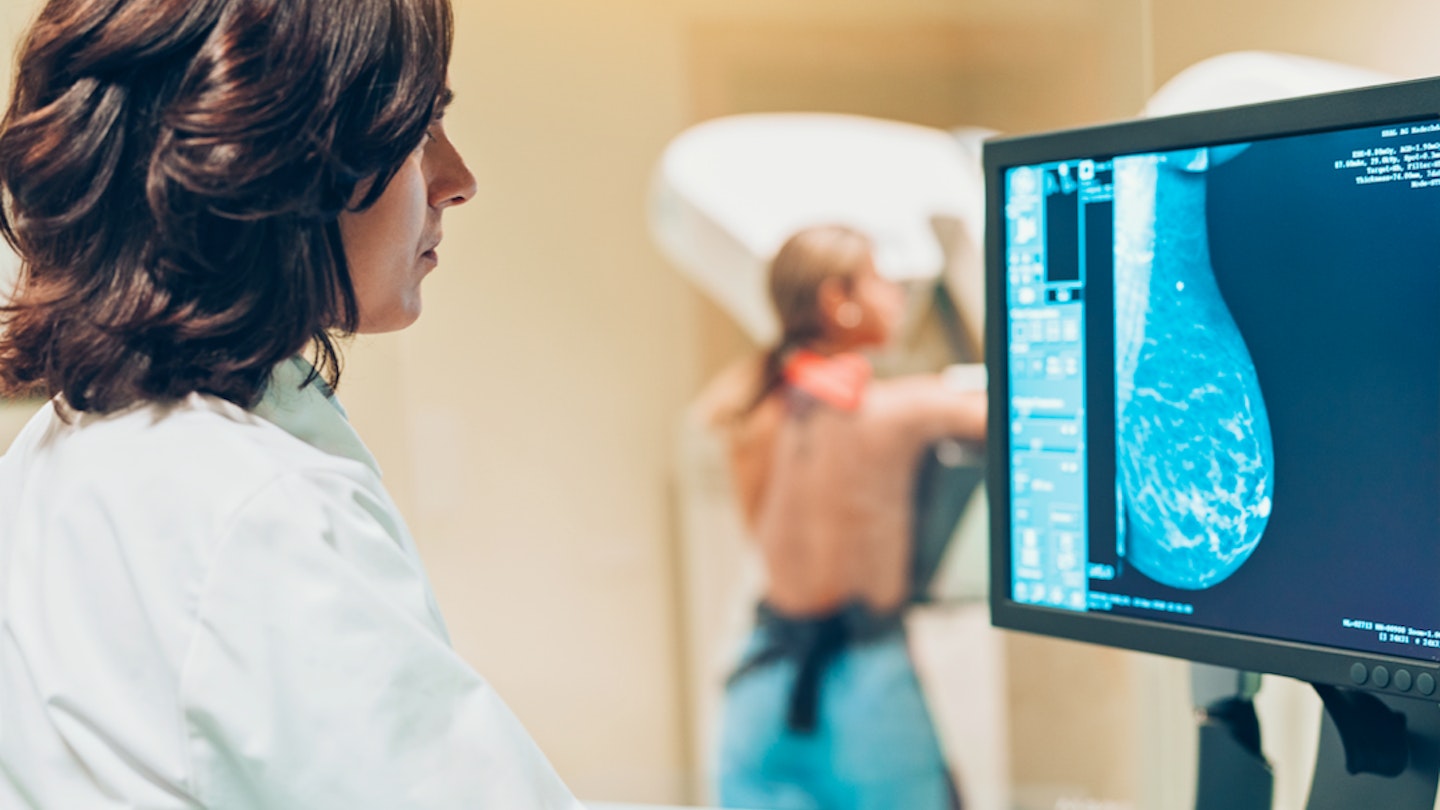
1. Since late July, breast cancer screening has restarted so women will be receiving invitations again. The process of attending and having scans has been adapted to allow extra time for cleaning between visits and to ensure sufficient space for social distancing. If you are overdue a mammogram or are invited to attend, you can do so knowing that all necessary precautions are being taken for your safety. In England, breast cancer screening is offered to women aged 50 to 71, but you may be eligible for a mammogram / MRI if you have a very high risk of developing cancer.
2. Diagnosis usually involves attendance at a one-stop clinic. This means being seen and examined by a breast specialist and then having the triple assessment of breast imaging; with an ultrasound, a mammogram and a biopsy, where a sample of tissue is removed to confirm the diagnosis. Now following a referral, you might have a telephone or video consultation first and then come in for necessary investigations after being assessed by a breast specialist. If surgery is required, then this will be in a COVID secure environment but will mean a period of isolation and a COVID test before going into hospital. The types of surgery you will be offered is likely to be the same as pre-COVID currently. During the height of the initial pandemic, surgery was being kept as safe as possible by limiting complex surgery, which includes many types of breast reconstruction for those women having a mastectomy. If a reconstruction was not possible for you initially this is surgery which can be offered later.
During the first wave of the pandemic, treatments were prioritised to ensure that anyone receiving curative treatment with chemotherapy continued treatment as safely as possible. Again, the UK government put in place a process of ‘shielding’ which lasted throughout the initial lockdown and beyond. This was really restrictive and many patients found this extremely hard, facing treatment and its impact whilst being alone and isolated.
However, clinical consultations are still being done by telephone and/or video and the importance of the breast care nursing teams in providing additional support is invaluable, especially as visitors either accompanying patients or visiting in-patients is still very restricted. Some treatments were reduced in duration or frequency which in the curative setting were done when it was considered safe to do so. This includes the duration of some radiotherapy treatments.
For those patients who were receiving palliative chemotherapy, unfortunately the risks of treatment were considered too great and some treatments were stopped. Initial data suggested that patients on chemotherapy had excess mortality from coronavirus, but now we have more data and the risks of treatment versus the benefits will be discussed by your medical team.
Although cancer services are different it is so important to emphasise that diagnosis and treatment is ongoing and if you are worried about any breast changes you should contact your GP who will refer you urgently. The same teams that would have provided treatment pre-COVID will be available to support you through treatment now. Don’t wait. Contact your doctor. Get checked.